Celiac Disease
Understanding Celiac Disease
Celiac Disease (CD) is a chronic digestive disorder characterized by inflammation of the small intestine, impacting nutrient absorption. This condition is triggered by the consumption of gluten, a protein found in wheat, barley, rye, and related grains. While oats are generally considered safe, the risk of contamination limits their recommended intake for those with CD.
Disease Mechanism & Progression
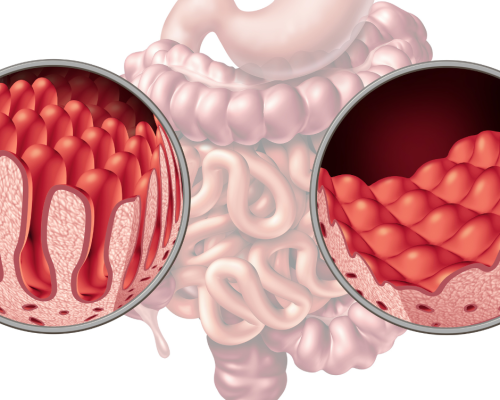
Upon gluten ingestion, the immune system initiates an inflammatory response in the small intestine, damaging millions of finger-like projections called villi. These structures, crucial for nutrient absorption, become compromised, leading to decreased nutrient assimilation. Eliminating gluten from the diet reduces inflammation, allowing the intestine to heal gradually.
The onset of symptoms varies among individuals, with some experiencing effects decades after initial gluten exposure. Triggers can precipitate symptoms and signs, making the disease presentation diverse.

Prevalence of Celiac Disease
In the United States, an estimated 1 in 100 people may have CD, yet only 1 in 5 are diagnosed. CD spans various ethnicities, with Caucasians having the highest prevalence. While it can manifest in infancy, diagnosis often occurs in adulthood, with a higher incidence in females. Those with type 1 diabetes, thyroid disorders, or family history face an increased risk.

Symptoms of Celiac Disease
Symptoms vary widely, from mild inflammation with minimal signs to severe cases prompting medical attention. Common symptoms include abdominal pain, bloating, diarrhea, weight loss, anemia, and poor growth in children. CD can mimic other conditions, necessitating screening for patients with symptoms resembling irritable bowel syndrome.
Treatment Strategies
The primary treatment for CD is adherence to a gluten-free diet, promoting intestinal healing. Dieticians play a crucial role in educating patients and tailoring gluten-free diets. Medications are rarely needed, except in cases where a gluten-free diet is ineffective. Support groups offer valuable resources for patients and their families.
- Gluten-Free Diet Guidelines: Avoiding gluten-containing grains like wheat, barley, rye, and related products is imperative. Patients must be vigilant label readers, identifying and eliminating potentially harmful ingredients. Certain grains and flours, labeled gluten-free, are safe alternatives.
- Lifelong Commitment: Once diagnosed, individuals must maintain a strict gluten-free diet throughout their lives. While the transition may be challenging initially, dieticians provide valuable support.
- Complications and Follow-Up: Non-adherence to the gluten-free diet leads to persistent symptoms and an increased risk of complications, including cancer and intestinal narrowing. Annual follow-ups, including blood tests and potential endoscopy, ensure ongoing healing and symptom resolution.
- Family Involvement: Given the genetic nature of CD, immediate family members should undergo testing, even if asymptomatic, to detect potential hidden cases
In conclusion, understanding Celiac Disease involves recognizing its diverse symptoms, adhering to diagnostic protocols, and committing to a lifelong gluten-free lifestyle. Regular follow-ups and family involvement are integral components of managing this chronic digestive disorder.
